
If you think colon cancer is a man’s disease, that only older people get it and that it cannot be prevented, you have fallen for three common myths related to the third most diagnosed cancer in the United States. Instead, you should know it affects young men and women alike, its incidence is growing among adults under 50 and it’s one of those cancers that run in families.
March is Colon Cancer Awareness Month and a good time to get your facts straight. According to the American Cancer Society (ACS), some 143,000 people will be diagnosed with colorectal cancer in 2013, when it is expected to cause more than 50,800 deaths. The chances of developing colorectal cancer during your lifetime are currently estimated at 1 in 20. Maybe you don’t have anybody close to you with this disease or, like me, you have lost a relative to colon cancer—but in any case, listen up and be informed!
Read Related: Breast Cancer Awareness Month: My First as a Patient
THE BASICS
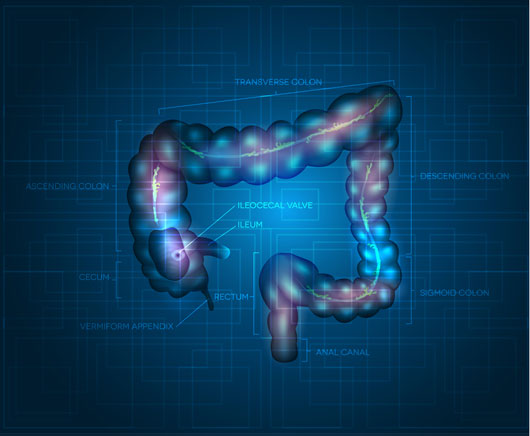
The colon is the last part of our digestive system, a 5-foot long muscular tube, also called the large intestine. Water and salt from our food are absorbed by the colon after the small intestine has done the same with most of the nutrients. The last six inches of the colon are called the rectum. Cancer in the colon and rectum share many features, which is why it is generally referred to as colorectal cancer.
Cancer usually starts in the inner layer of the colon in the form of a benign polyp. This is an elevated growth that can be discovered with an imaging test. Over time, this abnormal tissue can develop into cancer. Other digestive conditions that cause chronic inflammation of the colon affect the lining and can also develop into cancer.
Colorectal cancer tends to grow slowly, over a period of years. If cancer begins to form in polyps, or in the cells of the lining, it will grow into the wall of the colon, eventually reaching blood and lymph vessels. At this point, it can spread to distant organs causing metastasis. Colorectal cancer most commonly spreads to the liver and lungs. For complete information on different types of colorectal cancer, check the American Cancer Society.

KNOW YOUR RISK
While colorectal cancer may run in families, family history explains only about 20% of cases. As with other types of cancer, it is often difficult to pinpoint the trigger. Known risk factors for colorectal cancer include:
Age: Odds increase with age to the extent that almost 90% of patients diagnosed are over 50 years old. Younger cases usually have additional risk factors.
Inflammatory Bowel Disease: Having IBD over a long period of time increases the risk, since chronic inflammation is a known trigger of cancer. IBD includes Crohn’s disease and ulcerative colitis.
Family History: Those who have one first-degree relative with colorectal cancer are at twice the risk of developing this disease. If this family member was younger than 45 or if more relatives are affected, the chances are even greater.
Inherited Syndromes: Several hereditary genetic mutations multiply the risk of colorectal cancer, which usually develops at a younger age when this is the cause. Other types of cancer may be linked to these syndromes, so it is crucial to learn as much as possible about your family’s health history, including distant relatives.
Type 2 Diabetes: People with type 2 diabetes are more likely to develop colorectal cancer.
Lifestyle Factors: Studies point to diets high in processed meats and red meat as a cause of colorectal cancer; similarly, diets low in calcium, folate and fiber are also linked to a higher risk. Obesity and inactivity are believed to be associated with an increased risk, as is smoking and heavy alcohol consumption.
Previous History: People who have been affected by colorectal cancer or colon polyps in the past are more likely to develop this cancer. Women with a history of cancer of the breast, ovaries or endometrium are also at a higher risk.

SYMPTOMS & SCREENING
The initial stages of colorectal cancer usually do not present any symptoms, but as the disease progresses, some characteristic signs may appear. Even though these same symptoms are associated with other conditions, you should see your doctor as soon as possible if you notice any abnormal changes, such as:
1. A change in bowel movements that persists for some time.
2. Blood in your stool or toilet bowl.
3. Persistent abdominal discomfort: cramps, bloating or pain.
4. Weight loss for unexplained reasons.
5. Weakness or fatigue.
To catch this disease early, doctors recommend regular screening starting at age 50 for those at average risk, and earlier for people with additional factors that may increase their chances of developing colorectal cancer. Colonoscopies are largely credited for the decline in death rates due to colorectal cancer in adults 50 and older. However about half the eligible population is not benefiting from this screening due to lack of awareness, limited health care access, or as a result of the perceived discomfort associated with these tests, among other reasons.
According to the National Cancer Institute, the survival rate when the cancer is diagnosed at a localized stage (it hasn’t spread from the initial location) is almost 90% after five years. If diagnosed at a regional stage, when it has infected nearby lymph nodes, five-year survival rate is approximately 69%. But when the diagnosis is made after colorectal cancer has metastasized, less than 11% of patients survive five years.
Imaging tests are designed to discover abnormal cells and polyps even before they turn into cancer. Screening methods, as explained by the Colon Cancer Alliance, include:
Colonoscopy: So far, the best screening method. Recommended every ten years starting at age 50.
Flexible Sigmoidoscopy: Examines only the lower part of the colon; every five years starting at age 50.
Virtual Colonoscopy: X-rays and computers take images of the colon; every five years starting at age 50.
Double-Contrast Barium Enema: Barium is used as a contrast to reveal any abnormalities on X-rays. Recommended every five or ten years starting at 50.

TAKE ACTION AGAINST CANCER
What can you do to protect your family from colorectal cancer? Our best bet to fend off this and other serious illnesses is to lead a healthy lifestyle. While this may not seem much of a strategy, the American Cancer Society (ACS) reports one third of all cancer deaths in the United States are linked to diet and physical inactivity. Another third is caused by tobacco products. Furthermore, the link between colorectal cancer, diet and sedentary lifestyle seems stronger than for other types of cancer.
Unlike genetics and other risk factors beyond our control, these habits are entirely up to us. Setting an example and educating our children to stay healthy is our responsibility. To learn more about the ACS Guidelines for Nutrition and Physical Activity for Cancer Prevention, visit Cancer.org.
During Colon Cancer Awareness Month, make it your cause to find out about your family’s health history; including grandparents, uncles, aunts and cousins. Take advantage of your next visit to the doctor to discuss any serious illnesses that affect your relatives. Remember, information is the key to prevention!











